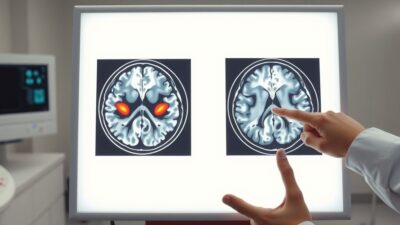
Over 450,000 U.S. service members have been diagnosed with traumatic brain injury since 2000, the vast majority classified as mild TBI from blast exposure. Despite multiple Department of Defense-funded trials showing cognitive improvement with HBOT at 1.5 ATA, the VA does not cover hyperbaric oxygen therapy for TBI outside of research protocols. A 2020 RCT by Harch et al. found significant improvement in post-concussion symptoms, PTSD scores, and cognitive function in military veterans after 40 HBOT sessions. Access remains the central barrier, not evidence. It is one of several neurological conditions studied alongside HBOT currently being explored in clinical research.
Blast-related TBI: a different kind of brain injury
Military traumatic brain injury is predominantly blast-induced, and blast TBI differs from civilian concussion in ways that matter for treatment. The Defense and Veterans Brain Injury Center (now the TBI Center of Excellence) has tracked over 450,000 TBI diagnoses in the U.S. military since 2000. Approximately 82% are classified as mild TBI. The actual number is almost certainly higher, since many blast exposures go unreported or undiagnosed in theater.
A blast wave produces a unique injury pattern. The primary blast wave (the pressure wave from the explosion) passes through the skull and creates shearing forces across the entire brain simultaneously. This differs from blunt-force concussion, where focal impact produces localized injury. The result is a more diffuse pattern of axonal damage, microhemorrhage, and neuroinflammation that affects multiple brain regions at once.
Blast TBI also carries a high co-occurrence with post-traumatic stress disorder. A 2013 study in JAMA Psychiatry found that repetitive blast TBI in deployed personnel was independently associated with increased PTSD symptoms and suicidal ideation. The overlap between PCS and PTSD symptoms (sleep disturbance, irritability, concentration problems, memory deficits) makes both diagnosis and treatment complicated. Treating one without addressing the other often produces incomplete results.
Standard VA treatment for mild TBI follows the VA/DoD Clinical Practice Guideline: symptom management with medication, cognitive rehabilitation, psychotherapy, and graded return to activity. For many veterans, these interventions help. For those with persistent symptoms, the options within the VA system narrow considerably.
DOD-funded HBOT trials: what they found
The Department of Defense has funded several controlled trials of HBOT for military TBI over the past 15 years. The results collectively show cognitive and symptomatic improvement, but the interpretation of these results has been contentious.
The Harch et al. 2020 trial in Medical Gas Research randomized military veterans with mild TBI and persistent postconcussion symptoms to HBOT at 1.5 ATA or sham. Forty sessions were administered. The HBOT group showed statistically significant improvements in postconcussion symptoms (RPQ scores), PTSD symptoms (PCL-M scores), and cognitive testing (working memory, processing speed). SPECT imaging confirmed improved cerebral blood flow in the treatment group.
The Cifu et al. 2014 study, funded by the DoD, compared HBOT at 2.0 ATA, HBOT at 1.5 ATA, and sham air at 1.3 ATA in active duty service members with persistent postconcussion symptoms. All three groups improved. The authors concluded that HBOT showed no benefit over sham. Critics, including Harch, argued that the “sham” at 1.3 ATA was itself a therapeutic dose of pressurized oxygen, making the comparison invalid. This debate has never been fully resolved and sits at the center of the VA coverage controversy.
A 2021 analysis by Biggs et al. in the Journal of Applied Physiology examined effect sizes across multiple military HBOT TBI trials. They found medium to large effect sizes for both symptomatic and cognitive improvements, even in studies that reported negative primary outcomes. The discrepancy between effect sizes and study conclusions reflects methodological disagreements about sham controls, not about whether patients actually improved.
The 2025 Weaver et al. trial in Scientific Reports added to the picture with a rigorous double-blind design. HBOT at 1.5 ATA showed improvement over sham, though the sham group also improved. The pattern is consistent: patients receiving HBOT get better, sham patients also get better (likely because the sham provides some pressurization), and the between-group differences, while present, are smaller than the within-group improvements.
Why the VA does not cover HBOT for TBI
The VA’s position on HBOT for TBI rests on three pillars, each of which has been challenged by HBOT advocates.
FDA indication: HBOT is not FDA-cleared for TBI. The FDA has cleared HBOT for 14 specific conditions (including air embolism, carbon monoxide poisoning, and non-healing wounds), and TBI is not among them. The VA generally follows FDA indications for treatment coverage. HBOT for TBI is classified as “off-label,” which does not mean prohibited but does mean not reimbursed through standard channels.
Sham control debate: VA clinical leadership has cited the DoD-funded trials (particularly Cifu 2014) as evidence that HBOT does not outperform sham for TBI. The counterargument (that 1.3 ATA air is not a true sham because any pressurization above 1.0 ATA increases tissue oxygenation) has been published in peer-reviewed journals but has not changed VA policy.
Cost and scalability: Providing HBOT to even a fraction of the 450,000+ veterans with TBI diagnoses would require massive infrastructure investment. The VA has approximately 25 HBOT-capable facilities, concentrated at major medical centers. Expanding this to meet potential demand would cost hundreds of millions of dollars. This practical constraint, while rarely stated explicitly, influences policy decisions.
A 2025 Department of Defense information paper reviewed the cumulative evidence and acknowledged that HBOT shows promise for mild TBI but concluded that “additional well-designed trials are needed before a definitive recommendation can be made.” The paper recommended continued funding for the HOBIT (Hyperbaric Oxygen Brain Injury Treatment) adaptive trial, which is evaluating optimal dosing protocols for severe TBI.
Congressional efforts and the legislative landscape
Congressional interest in HBOT for veterans with TBI has been bipartisan and persistent. Multiple bills have been introduced to mandate VA coverage or funding for HBOT for TBI, though none have become law as of this writing.
The HBOT Access Act and similar legislative proposals would require the VA to provide or reimburse HBOT for veterans diagnosed with TBI or PTSD. These bills have garnered support from veteran service organizations, HBOT provider associations, and individual advocates (including several high-profile veterans who credit HBOT with their recovery).
The legislative efforts face opposition from the VA itself, which has consistently testified that the evidence does not support routine clinical use, and from skeptics within the military medical community who view the positive trial results as confounded by inadequate sham controls.
Some VA medical centers have begun offering HBOT for TBI through research protocols or individual clinical decisions. These are not standardized programs but rather case-by-case determinations by local clinicians. A veteran’s access to HBOT through the VA depends heavily on geography and the local medical center’s willingness to pursue the treatment.
Nonprofits and alternative access pathways
The gap between evidence and VA coverage has been partially filled by nonprofit organizations that fund HBOT for veterans. Several operate nationally, providing treatment at no cost to qualifying veterans.
The HBOT4Heroes Foundation provides funded HBOT sessions for veterans and first responders with TBI and PTSD. The organization partners with HBOT clinics across the country and covers session costs directly.
The International Hyperbaric Medical Foundation (IHMF) has conducted its own treatment programs for veterans and published outcomes data. Paul Harch, the researcher behind the 1.5 ATA protocol, is affiliated with this organization.
TreatNOW Coalition is an advocacy and treatment-access organization specifically focused on getting HBOT to veterans with TBI. They maintain a directory of clinics offering discounted or donated treatment for veterans.
Local VFW and American Legion posts in some areas have fundraised for individual veterans to receive HBOT, typically partnering with local clinics for reduced rates.
These organizations collectively provide HBOT to several thousand veterans per year, a fraction of the potential demand but a meaningful lifeline for individuals who cannot access or afford treatment otherwise. For a broader view of veteran access options, see our guide to HBOT for veterans.
The Harch protocol for military TBI
Paul Harch, a physician and researcher at Louisiana State University Health Sciences Center, has been the most prominent advocate for HBOT in TBI for over two decades. His protocol for military TBI has become the de facto standard in the HBOT community, though it has not been adopted by the VA.
The Harch protocol specifies:
- Pressure: 1.5 ATA (atmospheres absolute)
- Gas: 100% medical oxygen
- Duration: 60 minutes at pressure (approximately 90 minutes total with pressurization/depressurization)
- Frequency: Five sessions per week
- Total sessions: 40, with extension to 60 or 80 based on clinical response
The 1.5 ATA pressure point is central to Harch’s argument and is supported by his 2022 systematic review in Frontiers in Neurology. The review analyzed all published HBOT TBI studies by pressure and concluded that 1.5 ATA produced consistently positive results while pressures at or above 2.0 ATA showed diminishing or no benefit. The proposed mechanism: 1.5 ATA increases tissue oxygenation enough to trigger neuroplasticity and angiogenesis without the vasoconstriction that higher pressures cause.
Harch also uses SPECT brain imaging before and after treatment as both a diagnostic and monitoring tool. Pre-treatment SPECT scans typically show regions of reduced blood flow corresponding to the patient’s symptom profile. Post-treatment scans show improvement in these regions, providing an objective measure of treatment response. The correlation between SPECT changes and symptom improvement has been documented across his published trials.
Critics note that the Harch protocol has been tested primarily in studies where Harch was the principal investigator, and that independent replication with equally rigorous methodology is limited. The 2025 Weaver study used 1.5 ATA independently and found positive results, which partially addresses this concern. For the full evidence landscape, see our HBOT for TBI clinical data review.
Cost and practical considerations for veterans
Without VA coverage, veterans seeking HBOT for TBI face significant financial and logistical barriers. Understanding these upfront is important for managing expectations and planning treatment.
Cost: A 40-session protocol at a private HBOT clinic runs $6,000 to $16,000 depending on location and facility type. Some clinics offer military discounts (10% to 25%). Package pricing is common. Financing through medical credit companies (CareCredit, Prosper Healthcare Lending) is available at some facilities.
Insurance: TRICARE does not cover HBOT for TBI. The VA does not cover it outside research protocols. Some private insurance plans that veterans may carry through civilian employment will cover HBOT for FDA-approved indications but deny claims for TBI. For more on the insurance landscape, see our HBOT insurance coverage guide.
Time commitment: Five sessions per week for eight weeks requires significant schedule restructuring. Veterans who are employed, in school, or caring for family members face real logistical challenges. Remote or rural veterans may face multi-hour drives to the nearest HBOT facility.
Documentation: Veterans considering future VA claims related to TBI should document their HBOT treatment, including pre and post assessments. If VA policy changes to cover HBOT for TBI (which legislative efforts aim to achieve), documented prior treatment may support retroactive claims.
Sources
- Harch PG, Andrews SR, Rowe CJ, et al. “Hyperbaric oxygen therapy for mild traumatic brain injury persistent postconcussion syndrome: a randomized controlled trial.” Medical Gas Research. 2020;10(1):8-20. DOI: 10.4103/2045-9912.279978
- Cifu DX, et al. “The Effect of Hyperbaric Oxygen on Persistent Postconcussion Symptoms.” Journal of Head Trauma Rehabilitation. 2014;29(1):11-20. DOI: 10.1097/HTR.0b013e3182a6aaf0
- Weaver LK, Ziemnik R, Deru K, Russo AA. “A double-blind randomized trial of hyperbaric oxygen for persistent symptoms after brain injury.” Scientific Reports. 2025;15. DOI: 10.1038/s41598-025-86631-6
- Biggs AT, Dainer H, Littlejohn LF. “Effect Sizes for Symptomatic and Cognitive Improvements in Traumatic Brain Injury Following Hyperbaric Oxygen Therapy.” Journal of Applied Physiology. 2021. DOI: 10.1152/japplphysiol.01084.2020
- Harch PG. “Systematic Review and Dosage Analysis: Hyperbaric Oxygen Therapy Efficacy in Mild Traumatic Brain Injury Persistent Postconcussion Syndrome.” Frontiers in Neurology. 2022;13:815056. DOI: 10.3389/fneur.2022.815056
- Bryan CJ, Clemans TA. “Repetitive traumatic brain injury, psychological symptoms, and suicide risk in a clinical sample of deployed military personnel.” JAMA Psychiatry. 2013;70(7):686-691. DOI: 10.1001/jamapsychiatry.2013.1093
- Defense and Veterans Brain Injury Center. “DoD TBI Worldwide Numbers.” TBI Center of Excellence. health.mil
- Boussi-Gross R, Golan H, Fishlev G, et al. “Hyperbaric oxygen therapy can improve post concussion syndrome years after mild traumatic brain injury.” PLoS One. 2013;8(11):e79995. DOI: 10.1371/journal.pone.0079995
- Hadanny A, Catalogna M, Yaniv S, et al. “Hyperbaric oxygen therapy in children with post-concussion syndrome improves cognitive and behavioral function.” Scientific Reports. 2022;12:15233. DOI: 10.1038/s41598-022-19395-y
- Shahid S, et al. “HBOT for neurocognitive deficits following TBI: a systematic review and meta-analysis.” Annals of Medicine and Surgery. 2025. DOI: 10.1097/MS9.0000000000003902
Medical Disclaimer
The content on BaricBoost.com is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.