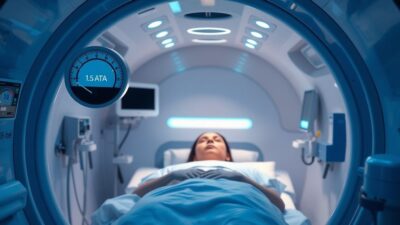
A 2022 randomized controlled trial by Hadanny et al. found that 60 sessions of HBOT at 1.5 ATA significantly improved cognitive function, behavioral symptoms, and quality of life in children aged 8 to 15 with post-concussion syndrome. The study enrolled 15 pediatric patients with persistent symptoms lasting at least six months. Results showed improvements in memory, attention, and executive function, confirmed by both neurocognitive testing and functional MRI changes. It is one of several HBOT for a range of brain and neurological conditions currently being explored in clinical research.
Concussion in children: different biology, different recovery
Children are not small adults when it comes to brain injury. The developing brain responds differently to concussion at every level. Pediatric concussions account for roughly 1.1 to 1.9 million cases annually in the United States among children under 18 (CDC estimates). The incidence has risen significantly over the past two decades, partly due to better recognition and reporting.
Recovery timelines diverge from adults. While most adult concussions resolve within 10 to 14 days, children and adolescents take longer. A 2014 JAMA Pediatrics study found that the median recovery time for children aged 5 to 18 was 28 days, roughly double the adult average. Approximately 25% to 30% of pediatric concussion patients develop persistent symptoms beyond three months.
The reasons are partly structural. The pediatric brain has higher water content, less myelination, and thinner cranial bones providing less protection. But the more concerning factor is developmental vulnerability. A concussion that disrupts normal neural development during critical windows (ages 8 to 15 especially) can have cascading effects on academic performance, social development, and emotional regulation that compound over time.
Standard pediatric concussion protocols emphasize cognitive and physical rest followed by graded return to school and activity. For the majority, this works. For children with persistent symptoms, the options narrow quickly. Stimulant medications for attention problems carry different risk profiles in developing brains. Antidepressants for mood symptoms are used cautiously given FDA black box warnings in pediatric populations.
The 2022 pediatric HBOT trial: what it found
The Hadanny et al. 2022 study published in Scientific Reports is the most rigorous controlled trial of HBOT in pediatric post-concussion syndrome to date. The study design, participant characteristics, and results deserve detailed examination because they form the foundation of the pediatric HBOT evidence base.
Study design: Prospective randomized controlled trial conducted at the Sagol Center for Hyperbaric Medicine and Research in Israel. Children aged 8 to 15 with diagnosed post-concussion syndrome lasting at least 6 months were enrolled. The treatment group received 60 daily HBOT sessions at 1.5 ATA with 100% oxygen for 60 minutes each.
Assessment tools: Researchers used a comprehensive battery including the Maudsley Attention and Response Suppression task (MARS), NeuroTrax computerized cognitive testing, the Post-Concussion Symptom Inventory (PCSI, both child and parent versions), and functional MRI to assess brain connectivity.
Cognitive results: The treatment group showed significant improvements in attention, processing speed, and executive function. The cognitive gains were measurable on standardized neuropsychological testing, not just parent-reported symptom scales. This distinction matters because parent reporting in pediatric studies is subject to expectation bias.
Behavioral results: Parents reported significant improvements in behavioral symptoms. Children showed reduced irritability, better emotional regulation, and improved sleep. Teacher reports (where available) corroborated the parental observations.
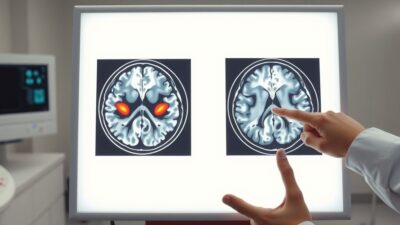
Imaging results: Functional MRI showed changes in brain connectivity patterns in the treatment group, providing an objective biological correlate for the reported improvements. Specific increases in connectivity were observed in frontal and temporal regions associated with attention and memory.
Limitations: The sample size was small (n=15 treatment). The study was conducted at a single center. Blinding was imperfect because sham HBOT in children raises ethical considerations. These limitations mean the results are promising but not definitive. Larger multi-center trials are needed.
Protocol for children: how it differs from adults
The pediatric HBOT protocol used in clinical trials and recommended by experienced practitioners shares core parameters with adult protocols but includes modifications for the developing brain and the practical realities of treating children.
Pressure: 1.5 ATA, identical to the adult PCS protocol. No pediatric-specific pressure modifications have been studied. Pressures above 2.0 ATA are avoided for brain injury indications regardless of age, based on the dosage analysis by Harch (2022).
Session duration: 60 minutes of oxygen breathing at pressure. Total chamber time is approximately 90 minutes including pressurization and depressurization. Some pediatric centers use shorter 45-minute sessions for younger children (under 10) who have difficulty remaining still.
Session count: The Hadanny trial used 60 sessions, more than the standard 40-session adult protocol. The rationale is that the developing brain may require more exposure to achieve comparable neuroplastic effects. Some practitioners start with 40 sessions and extend to 60 based on clinical response.
Frequency: Five sessions per week (Monday through Friday). This means a 60-session protocol takes 12 weeks. The schedule conflicts with school attendance, which is a practical barrier. Some families coordinate with schools for partial attendance or home instruction during treatment.
Supervision: A parent or guardian accompanies the child in the chamber. This is standard practice and serves both safety and comfort purposes. Monoplace chambers accommodate one patient, so the parent sits outside with visual contact. Multiplace chambers allow the parent to sit beside the child at pressure.
Ear equalization: Children sometimes have more difficulty equalizing ear pressure during pressurization than adults. Practitioners teach swallowing, jaw movement, and Valsalva techniques before the first session. For children who cannot equalize reliably, slower pressurization rates are used. Rarely, myringotomy tubes may be placed before starting HBOT, a minor procedure that eliminates the equalization requirement.
Safety: what the evidence shows for pediatric HBOT
The safety profile of HBOT in children is well-documented across multiple indications, not just concussion. HBOT has been used in pediatric patients for decades for conditions including carbon monoxide poisoning, decompression illness, and radiation injury. The pediatric HBOT safety literature consistently shows a low adverse event rate.
Common side effects in children mirror those in adults: middle ear discomfort during pressurization (the most frequent complaint, occurring in approximately 15% to 20% of pediatric patients), mild fatigue after sessions, and temporary myopia (nearsightedness) that resolves within weeks of completing treatment.
Serious adverse events are rare. Oxygen toxicity seizures, the most feared complication, occur at a rate of approximately 1 in 10,000 sessions at pressures below 2.0 ATA. At 1.5 ATA (the PCS protocol pressure), the risk is lower still. No oxygen toxicity seizures were reported in the Hadanny 2022 pediatric trial.
Contraindications in children are the same as in adults: untreated pneumothorax, certain chemotherapy agents (bleomycin, cisplatin, doxorubicin), and inability to equalize ear pressure that cannot be resolved with tubes. Active seizure disorders require careful evaluation but are not absolute contraindications.
The psychological impact of the treatment environment deserves mention. A hyperbaric chamber can be intimidating for children, particularly younger ones. The enclosed space, the sounds of pressurization, and the duration of sessions require preparation. Centers experienced in pediatric HBOT use familiarization visits, allow children to bring tablets or books, and ensure the child understands what will happen before the first session.
When to consider HBOT for a child with persistent concussion symptoms
HBOT is not a first-line treatment for pediatric concussion. Standard rest and graded return-to-activity protocols should be followed first. HBOT enters the conversation when symptoms persist beyond three to six months despite appropriate management. For context on HBOT and concussion more broadly, including how this fits into the wider treatment landscape, see our concussion overview.
Specific circumstances that may warrant consideration:
- Persistent cognitive symptoms (poor concentration, memory problems, processing speed deficits) that interfere with school performance after at least three months
- Chronic post-concussion headaches that have not responded to standard pharmacological and non-pharmacological management
- Behavioral or emotional changes (increased irritability, anxiety, emotional dysregulation) that emerged after the concussion and have not resolved
- Multiple concussions with cumulative symptom burden
Before pursuing HBOT, a thorough evaluation should rule out other treatable causes of persistent symptoms. Vestibular dysfunction, cervical spine injury, sleep disorders, and pre-existing conditions (ADHD, anxiety, learning disabilities) can mimic or worsen post-concussion symptoms. A pediatric neurologist or sports medicine physician experienced with concussion should complete this evaluation.
Parents should also understand the practical commitment. Twelve weeks of daily sessions means transportation, school accommodation, and cost. At $150 to $300 per session, a 60-session protocol runs $9,000 to $18,000 out of pocket. Insurance coverage for pediatric HBOT for concussion is rare. For more on what HBOT looks like for younger patients, see our guide to HBOT for children.
What the research still needs to answer
The pediatric HBOT evidence base for concussion is early-stage. The Hadanny 2022 trial provides the strongest signal, but several questions remain open.
Optimal session count: Is 60 sessions necessary, or would 40 produce equivalent results? No head-to-head comparison exists. The additional 20 sessions add cost, time, and missed school days. For a deeper look at the data behind the TBI evidence, see our HBOT for TBI data review.
Age effects: Does HBOT work differently in a 9-year-old versus a 15-year-old? The developmental stage of the brain at the time of injury and treatment likely matters, but no age-stratified analysis has been published.
Long-term durability: The Hadanny trial assessed outcomes at the end of treatment. Whether gains persist at 6, 12, or 24 months is unknown. This is particularly important in children, where the brain continues to develop and symptoms may evolve independent of treatment.
Optimal timing: Should HBOT be started at three months post-injury? Six months? A year? Starting earlier might prevent the entrenchment of maladaptive neural patterns, but starting too early might interfere with natural recovery. No trial has compared different treatment windows.
Combination therapy: Would HBOT paired with cognitive rehabilitation, neurofeedback, or graded exercise produce better results than HBOT alone? The multimodal approach seems logical but has not been tested in pediatric PCS.
Until these questions are answered by larger, multi-center trials, HBOT for pediatric PCS remains a treatment with a plausible mechanism, a positive signal from controlled trials, and a favorable safety profile, but without the depth of evidence needed for widespread clinical adoption or insurance coverage.
Sources
- Hadanny A, Catalogna M, Yaniv S, et al. “Hyperbaric oxygen therapy in children with post-concussion syndrome improves cognitive and behavioral function.” Scientific Reports. 2022;12:15233. DOI: 10.1038/s41598-022-19395-y
- Zemek R, Barrowman N, Freedman SB, et al. “Clinical risk score for persistent postconcussion symptoms among children with acute concussion in the ED.” JAMA. 2016;315(10):1014-1025. DOI: 10.1001/jama.2016.1203
- Barlow KM, Crawford S, Stevenson A, et al. “Epidemiology of postconcussion syndrome in pediatric mild traumatic brain injury.” Pediatrics. 2010;126(2):e374-e381. DOI: 10.1542/peds.2009-0925
- Harch PG. “Systematic Review and Dosage Analysis: Hyperbaric Oxygen Therapy Efficacy in Mild Traumatic Brain Injury Persistent Postconcussion Syndrome.” Frontiers in Neurology. 2022;13:815056. DOI: 10.3389/fneur.2022.815056
- Bryan CJ, Clemans TA. “Repetitive traumatic brain injury, psychological symptoms, and suicide risk in a clinical sample of deployed military personnel.” JAMA Psychiatry. 2013;70(7):686-691. DOI: 10.1001/jamapsychiatry.2013.1093
- Davis GA, Anderson V, Babl FE, et al. “What is the difference in concussion management in children as compared with adults? A systematic review.” British Journal of Sports Medicine. 2017;51(12):949-957. DOI: 10.1136/bjsports-2016-097415
- Boussi-Gross R, Golan H, Fishlev G, et al. “Hyperbaric oxygen therapy can improve post concussion syndrome years after mild traumatic brain injury.” PLoS One. 2013;8(11):e79995. DOI: 10.1371/journal.pone.0079995
- Rivara FP, Koepsell TD, Wang J, et al. “Incidence of disability among children 12 months after traumatic brain injury.” American Journal of Public Health. 2012;102(11):2074-2079. DOI: 10.2105/AJPH.2012.300696
Medical Disclaimer
The content on BaricBoost.com is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.