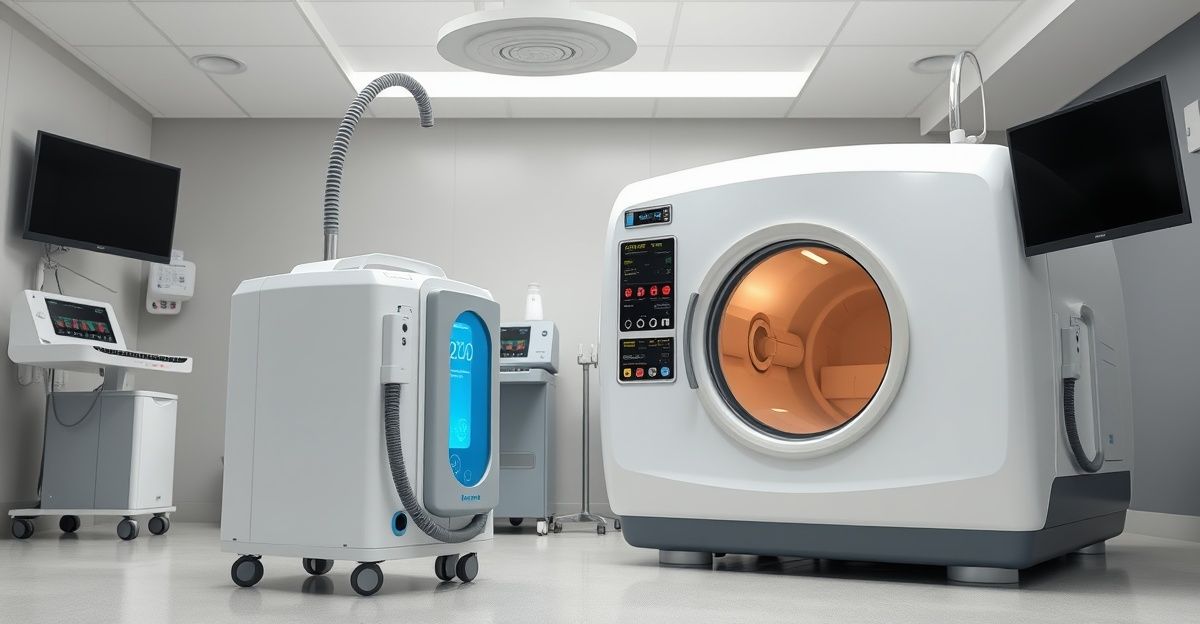
Combining hyperbaric oxygen therapy (HBOT) with negative-pressure wound therapy (NPWT, commonly known as wound VAC) targets two different barriers to chronic wound healing simultaneously. HBOT addresses tissue hypoxia by saturating wound tissue with dissolved oxygen at 10-15 times normal levels. Wound VAC addresses the wound surface environment by removing excess fluid, reducing edema, and mechanically stimulating granulation tissue growth. A 2019 retrospective study in Wounds found that patients receiving both therapies had faster wound closure times than those receiving either treatment alone. This is one of several HBOT applications in recovery and rehabilitation gaining attention in clinical practice.
What Is Negative-Pressure Wound Therapy (Wound VAC)?
A wound VAC (Vacuum-Assisted Closure) device applies controlled sub-atmospheric pressure to a wound bed through a sealed foam dressing connected to a portable suction unit. The FDA cleared the first wound VAC device (KCI V.A.C.) in 1995, and the technology has become standard care for complex wounds in hospitals and home settings. Over 7 million wound VAC units have been used in the US since introduction.
The wound VAC works through four primary mechanisms:
- Fluid removal: Continuous or intermittent suction removes wound exudate, infectious material, and inflammatory mediators (matrix metalloproteinases, TNF-alpha, IL-1) that inhibit healing
- Edema reduction: Negative pressure draws excess interstitial fluid away from the wound bed and surrounding tissue, decompressing capillary beds and improving microcirculation
- Macrodeformation: The foam dressing draws wound edges inward, mechanically reducing wound size by approximately 2-5% per dressing change in responsive wounds
- Microdeformation: Cellular-level mechanical stress at the foam-tissue interface stimulates fibroblast and endothelial cell proliferation through mechanotransduction pathways
Standard wound VAC settings use -125 mmHg of continuous or intermittent pressure. The device is worn 22-24 hours per day, with dressing changes every 48-72 hours. Most modern wound VAC devices are portable (weighing 1-3 pounds) and battery-powered, allowing patients to continue daily activities while maintaining negative-pressure therapy. Common devices include the KCI V.A.C. Ulta, Smith+Nephew RENASYS, and Cardinal Health NPWT systems.
Why HBOT and Wound VAC Target Different Problems
The rationale for combining these therapies is that they address complementary, non-overlapping barriers to healing. Understanding what each therapy does (and does not do) clarifies why they work well together.
HBOT solves the oxygen problem. Chronic wounds are hypoxic. Damaged or diseased microvasculature cannot deliver enough oxygen to support fibroblast collagen synthesis (which requires oxygen tension above 20 mmHg), neutrophil bacterial killing (which requires above 30-40 mmHg), or angiogenesis signaling (which paradoxically requires the steep oxygen gradient between hyperoxygenated blood and hypoxic tissue). HBOT forces dissolved oxygen into plasma at levels sufficient to diffuse into hypoxic tissue, independent of hemoglobin delivery.
Wound VAC solves the surface environment problem. Even in a well-oxygenated wound, healing stalls if the wound bed is bathed in exudate filled with proteases (MMP-2, MMP-9) that degrade new collagen as fast as fibroblasts produce it. Chronic wound fluid contains up to 8 times the protease levels of acute wound fluid, according to research published in the International Wound Journal. Wound VAC physically removes this hostile fluid, shifting the biochemical environment from degradation to synthesis.
Neither therapy replaces the other. A wound that is both hypoxic and chronically inflamed needs both the oxygen delivery that HBOT provides and the environmental optimization that wound VAC provides. This is why the combination is increasingly used at Level I and II wound care centers for the most refractory cases.
What Does the Research Say?
Direct head-to-head evidence comparing HBOT alone, wound VAC alone, and the combination remains limited but growing. Most evidence comes from retrospective analyses and case series at multidisciplinary wound care centers.
A 2019 retrospective study published in Wounds examined 89 patients with chronic diabetic foot ulcers treated at a multidisciplinary wound center. Patients receiving combined HBOT + NPWT achieved complete wound closure in a median of 8.2 weeks, compared to 12.4 weeks for HBOT alone and 14.1 weeks for NPWT alone. The combination group also had lower rates of wound recurrence at 6 months (12% vs. 24% for single-modality treatment).
Kessler et al. (2003) published a case series in Diabetes Care demonstrating that HBOT combined with aggressive wound management (including NPWT when indicated) produced healing rates of 76% in Wagner grade III-IV diabetic foot ulcers that had failed prior treatment. While this study did not isolate the NPWT component, it supports the multimodal approach.
A 2015 Cochrane review of NPWT for leg ulcers found that negative-pressure therapy improved healing compared to standard dressings, though evidence quality was low to moderate. The review did not specifically examine NPWT + HBOT combinations, highlighting a gap in the evidence that future trials need to address.
The biological rationale is supported by laboratory studies showing that HBOT-induced oxygen elevation enhances the wound VAC’s mechanotransduction effects. Cells under mechanical stress from negative pressure require adequate oxygen to respond with proliferation rather than apoptosis. Hypoxic cells stressed by NPWT may actually undergo programmed cell death rather than proliferate, which could explain why wound VAC alone sometimes fails in severely ischemic wounds with TCOM values below 20 mmHg.
How to Schedule HBOT and Wound VAC Together
The practical logistics of combining HBOT and wound VAC require coordination between the hyperbaric facility and the wound care team. Here is the typical scheduling approach:
Daily schedule:
- Wound VAC runs continuously 22-24 hours per day at the patient’s home or hospital room
- HBOT session once daily, 90 minutes at 2.0-2.4 ATA at the hyperbaric facility
- Wound VAC dressing is temporarily removed before the HBOT session (the VAC unit and its electrical components cannot enter the hyperbaric chamber due to fire and explosion risk in the enriched oxygen environment)
- A simple non-adherent dressing (Adaptic, Mepitel, or similar) covers the wound during the HBOT session
- Wound VAC dressing is reapplied immediately after HBOT, typically by the wound care nurse at the hyperbaric facility or at the patient’s wound care clinic
Dressing change coordination:
Wound VAC dressings are typically changed every 48-72 hours. Coordinating these changes with HBOT sessions reduces total wound exposure time and the number of dressing applications. Many centers schedule formal wound VAC dressing changes to coincide with the pre-HBOT dressing removal on Monday, Wednesday, and Friday, so the wound is assessed, debrided if needed, photographed for documentation, and re-dressed with fresh VAC foam after the hyperbaric session. On intervening days, a simple lift-and-replace of the VAC dressing suffices.
Travel and logistics:
Portable wound VAC devices (KCI V.A.C. Via, Smith+Nephew PICO, Cardinal Health PRO) allow patients to maintain negative-pressure therapy during transport to and from HBOT sessions. The device is paused during the chamber session and restarted immediately afterward. Most patients can manage this independently once trained, though initial sessions may benefit from wound care nurse assistance with dressing removal and reapplication.
For more HBOT wound data, see our wound healing statistics page.
Which Wounds Benefit Most from the Combination?
The HBOT + wound VAC combination is most valuable for wounds that are both hypoxic (TCOM below 40 mmHg on room air) and producing excessive exudate. Typical candidates include:
- Large diabetic foot ulcers (Wagner III-IV): Deep, exudative wounds in patients with peripheral neuropathy and vascular compromise. These are the most common candidates for combination therapy.
- Post-surgical dehiscence: Surgical wounds that have separated, particularly in irradiated tissue or in patients with diabetes, obesity, or immunosuppression
- Post-debridement wounds: Large wound beds created by surgical debridement of necrotizing fasciitis or osteomyelitis, where significant tissue has been removed and the remaining wound bed is hypoxic
- Traumatic wounds with tissue loss: Crush injuries or degloving injuries with significant soft tissue defects requiring both oxygen support and surface management
- Wounds being prepared for grafting: Building a healthy, vascular granulation bed before split-thickness skin graft placement. The combination can reduce time-to-graft-readiness by 2-3 weeks compared to standard care alone
Wounds that are small (less than 2 cm diameter), superficial (limited to dermis), or not significantly hypoxic (TCOM above 40 mmHg on room air) may not benefit from the added complexity and cost of dual therapy. Standard wound care with appropriate dressings, or single-modality treatment, is usually sufficient for these cases.
What Are the Side Effects and Risks?
Both HBOT and wound VAC are generally well-tolerated, but the combination adds logistical complexity and cost that patients and providers should consider before starting:
Cost: Running both therapies simultaneously roughly doubles the treatment expense. Wound VAC supplies (foam, drapes, canisters) cost $100-200 per dressing change, and the device rental adds $50-100 per day. HBOT costs $150-450 per session depending on facility type and insurance status. Many insurance plans cover both therapies independently but require separate prior authorizations for each. Confirm coverage for both before starting. Combined out-of-pocket costs can reach $500-700 per week even with insurance.
Infection monitoring: The wound is exposed twice daily (once for VAC dressing removal before HBOT, once for reapplication after). Each exposure is a potential opportunity for contamination. Strict aseptic technique during dressing changes is essential, and wound culture should be obtained if signs of new infection develop (increased erythema, purulent drainage, fever, elevated WBC).
Bleeding risk: Wound VAC can occasionally cause bleeding, particularly in highly vascularized wounds, wounds near major vessels, or in patients on anticoagulation. HBOT’s enhancement of angiogenesis increases local vascularity over time, which may theoretically increase bleeding risk with NPWT. Monitoring for excessive bleeding in the VAC canister is standard practice. If blood output exceeds 50 mL per dressing change, the wound care team should reassess.
Patient burden: Daily HBOT sessions (90 minutes plus travel and preparation, typically 2-3 hours total) combined with a portable wound VAC (worn 24/7 with alarms, dressing changes, and canister emptying) creates a significant treatment burden. This regimen lasts 4-6 weeks for most patients. Compliance is a real concern, and treatment plans should account for the reality that some patients will struggle to maintain this intensive schedule. Social support, transportation assistance, and regular encouragement from the care team all improve adherence.
For a comprehensive overview of HBOT wound care, see our wound healing guide.
When to Consider Dual Therapy vs. Single Treatment
Not every chronic wound needs both HBOT and wound VAC. The decision to use combination therapy should be based on clinical assessment of the specific barriers preventing healing in each individual wound. A useful decision framework:
HBOT alone is appropriate when the primary problem is tissue hypoxia (low TCOM values) but the wound bed is clean, manageable in size, and not producing excessive exudate. Small to medium diabetic foot ulcers, radiation wounds, and chronic osteomyelitis often respond well to HBOT plus standard dressing changes without needing NPWT.
Wound VAC alone is appropriate when the wound has adequate oxygenation (TCOM above 40 mmHg) but is large, exudative, or needs mechanical contraction to reduce size before grafting. Post-surgical wounds with adequate blood supply but large tissue defects often respond well to NPWT without HBOT.
Combination therapy is appropriate when the wound has both documented hypoxia (TCOM below 40 mmHg) and characteristics that benefit from NPWT (large size, high exudate, need for wound bed preparation). This is the wound that has multiple simultaneous barriers to healing, and addressing only one barrier is insufficient.
Discuss the options with your wound care team. A wound care specialist experienced in both modalities can assess whether the added cost and logistical burden of combination therapy is justified by the expected clinical benefit for your specific wound.
Sources
- Kranke P, Bennett MH, et al. “Hyperbaric oxygen therapy for chronic wounds.” Cochrane Database of Systematic Reviews, 2015. PubMed
- Kessler L, Bilbault P, et al. “Hyperbaric oxygenation accelerates the healing rate of nonischemic chronic diabetic foot ulcers.” Diabetes Care, 2003. PubMed
- Dumville JC, Land L, et al. “Negative pressure wound therapy for treating leg ulcers.” Cochrane Database of Systematic Reviews, 2015. PubMed
- Orgill DP, Bayer LR. “Negative pressure wound therapy: past, present and future.” International Wound Journal, 2013. PubMed
- U.S. Food and Drug Administration. “Negative Pressure Wound Therapy Devices.” FDA.gov
- Muller-Stich BP, et al. “Negative-pressure wound therapy versus standard wound care on diabetic foot ulcers.” Diabetes Care, 2008.
- Trengove NJ, Stacey MC, et al. “Analysis of the acute and chronic wound environments: the role of proteases and their inhibitors.” Wound Repair and Regeneration, 1999. PubMed
Medical Disclaimer
The content on BaricBoost.com is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.