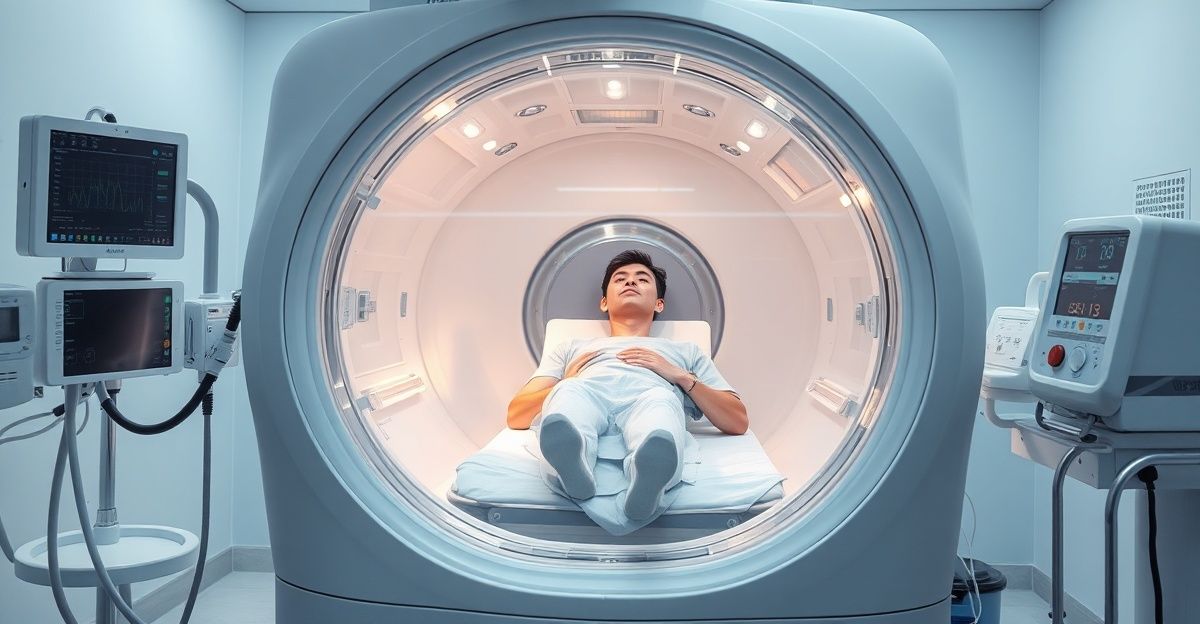
High-flow 100% oxygen is the immediate treatment for carbon monoxide poisoning, and HBOT is the standard of care for severe cases. CO poisoning kills roughly 400 Americans and sends 50,000 to the ER every year. The landmark Weaver 2002 RCT found HBOT reduced delayed neurological damage from 46.1% to 24.6%, with a number needed to treat (NNT) of 5. The clinical question is no longer whether HBOT works for severe CO poisoning, but how to identify which patients need it.
How Carbon Monoxide Damages the Body
Carbon monoxide binds to hemoglobin with 200 to 250 times the affinity of oxygen, forming carboxyhemoglobin (COHb). This does two things: it directly prevents hemoglobin from carrying oxygen, and it shifts the oxygen-hemoglobin dissociation curve to the left, making the remaining oxyhemoglobin hold onto its oxygen more tightly and release less to tissues.
But the damage goes beyond simple oxygen deprivation. CO also binds to myoglobin (affecting cardiac muscle function), cytochrome c oxidase (disrupting mitochondrial respiration), and causes direct oxidative damage to the central nervous system. This is why patients can still develop brain injury even after COHb levels normalize.
The brain and heart are the most vulnerable organs. Cardiac complications (arrhythmias, myocardial injury) are present in up to 37% of moderate-to-severe CO poisoning cases. Neurological damage ranges from headache and confusion in mild cases to coma, seizures, and permanent cognitive impairment in severe cases.
First-Line Treatment: 100% Normobaric Oxygen
Every patient with confirmed or suspected CO poisoning receives 100% oxygen via a tight-fitting non-rebreather mask as soon as possible. This is not optional and should not be delayed for any reason, including waiting for lab results.
The physics are simple: increasing inspired oxygen concentration from 21% (room air) to 100% accelerates the dissociation of CO from hemoglobin dramatically.
| Oxygen Delivery Method | CO Half-Life |
|---|---|
| Room air (21% O2) | 320 minutes (5.3 hours) |
| 100% O2, non-rebreather mask | 80 minutes (1.3 hours) |
| 100% O2, HBOT at 2.5-3.0 ATA | 23 minutes |
Treatment with normobaric 100% oxygen continues until COHb levels fall below 5% and symptoms resolve. In mild cases (brief exposure, no loss of consciousness, COHb below 15%), normobaric oxygen alone is often sufficient.
When HBOT Is Indicated
HBOT is an FDA-cleared indication for CO poisoning and is considered the standard of care for severe cases. The Undersea and Hyperbaric Medical Society (UHMS) recommends HBOT for CO poisoning meeting any of the following criteria:
- Loss of consciousness at any point during the exposure
- COHb level above 25% (or above 15% in pregnant patients)
- Neurological signs: confusion, ataxia, seizures, focal deficits
- Cardiac involvement: ischemia, arrhythmia, elevated troponin
- Pregnancy (fetal hemoglobin binds CO with even higher affinity than adult hemoglobin)
- Persistent symptoms after 4 to 6 hours of 100% normobaric oxygen
The Weaver Trial: The Landmark Study
The most influential study on HBOT for CO poisoning was published by Weaver et al. in the New England Journal of Medicine in 2002. This double-blind RCT randomized 152 patients with acute CO poisoning to either 3 sessions of HBOT or 3 sessions of normobaric oxygen over 24 hours.
The primary outcome was delayed neurological sequelae (DNS) at 6 weeks. Results were definitive:
- HBOT group: 24.7% developed DNS
- Control group: 46.1% developed DNS
- Absolute risk reduction: 21.4%
- Number needed to treat (NNT): 5 (meaning for every 5 patients treated with HBOT, one case of DNS is prevented)
The benefit persisted at 12-month follow-up. The HBOT group also showed better performance on cognitive testing, particularly in tests of attention, processing speed, and memory (Weaver et al., 2002).
“The Weaver trial changed practice. An NNT of 5 for preventing brain damage is exceptionally strong. The debate is no longer whether HBOT works for CO poisoning, but how quickly we can get patients into a chamber.”
What Does the HBOT Protocol Look Like?
The standard protocol, based on the Weaver trial and UHMS guidelines:
- First session: 3.0 ATA for 25 minutes, then 2.0 ATA for 90 minutes (total ~150 minutes), given as soon as possible after poisoning
- Second session: 2.0 ATA for 90 minutes, given 6 to 12 hours after the first
- Third session: 2.0 ATA for 90 minutes, given 6 to 12 hours after the second
- Total treatment: 3 sessions within 24 hours of poisoning
Timing is critical. HBOT appears to be most effective when the first session is delivered within 6 hours of CO exposure. Benefit diminishes beyond 24 hours, though some centers will treat patients up to 72 hours after exposure if they have persistent symptoms.
Delayed Neurological Sequelae (DNS)
DNS is the most feared complication of CO poisoning. After an initial period of apparent recovery (the “lucid interval”), patients develop new neurological symptoms 2 to 40 days later. The mechanism involves delayed demyelination, lipid peroxidation, and inflammatory damage in the white matter and basal ganglia.
Symptoms of DNS include:
- Memory impairment and difficulty concentrating
- Personality changes (apathy, irritability)
- Movement disorders (parkinsonian features)
- Gait disturbances
- Urinary incontinence
Without HBOT, DNS occurs in 25% to 46% of patients with significant CO exposure. With HBOT, this drops to 20% to 25%. In most cases, DNS resolves within 1 year, but approximately 25% of affected patients have persistent cognitive deficits.
Emergency Protocols and Practical Considerations
| Severity | Criteria | Treatment |
|---|---|---|
| Mild | COHb under 15%, brief exposure, headache only, no LOC | 100% O2 via NRB until COHb under 5% and symptom-free |
| Moderate | COHb 15-25%, prolonged exposure, confusion, no LOC | 100% O2 initially; consider HBOT, especially with cardiac or neuro symptoms |
| Severe | COHb above 25%, LOC, seizure, cardiac involvement, pregnancy | HBOT as soon as possible (3 sessions within 24 hours) |
| Critical | Coma, cardiovascular collapse | Intubation, 100% O2, emergent HBOT, ICU management |
A practical challenge: not every hospital has a hyperbaric chamber. In the US, roughly 1,200 HBOT facilities exist, but many are outpatient wound care centers not equipped for emergency treatment. Critical CO poisoning patients may need air transport to a center with 24/7 hyperbaric capability.
The Bottom Line
Carbon monoxide poisoning is one of the clearest indications for oxygen therapy in all of medicine. Normobaric 100% oxygen is life-saving and must be started immediately. For severe cases, HBOT reduces the half-life of carboxyhemoglobin from 80 minutes to 23 minutes and, more importantly, cuts the risk of delayed brain damage nearly in half. The Weaver trial remains one of the strongest pieces of evidence in hyperbaric medicine, with an NNT of 5 that few medical interventions can match. If you or someone you know is exposed to carbon monoxide, call 911 immediately and get to fresh air.
References
- Weaver, L. K., et al. (2002). Hyperbaric oxygen for acute carbon monoxide poisoning. New England Journal of Medicine, 347(14), 1057-1067. doi:10.1056/NEJMoa013121
- Rose, J. J., et al. (2017). Carbon monoxide poisoning: pathogenesis, management, and future directions of therapy. American Journal of Respiratory and Critical Care Medicine, 195(5), 596-606. doi:10.1164/rccm.201606-1275CI
- Hampson, N. B. (2018). Carboxyhemoglobin: A primer for clinicians. Undersea and Hyperbaric Medicine, 45(5), 523-528.
- Buckley, N. A., et al. (2011). Hyperbaric oxygen for carbon monoxide poisoning. Cochrane Database of Systematic Reviews, (4), CD002041. doi:10.1002/14651858.CD002041.pub3
- Thom, S. R. (2009). Oxidative stress is fundamental to hyperbaric oxygen therapy. Journal of Applied Physiology, 106(3), 988-995. doi:10.1152/japplphysiol.91004.2008
Medical Disclaimer
The content on BaricBoost.com is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.