Affiliate Disclosure
This article contains affiliate links. If you purchase through these links, we may earn a commission at no additional cost to you. This does not influence our evaluations or rankings.
Hyperbaric oxygen therapy increases oxygen delivery to damaged brain tissue by 10-15x normal levels, and clinical research shows measurable improvements in patients with traumatic brain injuries. A 2012 study of 56 TBI patients found significant cognitive gains after 40 HBOT sessions at 1.5 ATA, even years after injury. It is one of several brain and neurological conditions treated with HBOT currently being explored in clinical research.
If you’re dealing with a traumatic brain injury (TBI) or know someone who is, understanding how hyperbaric chambers work could open new doors for recovery. The research has moved quickly: a 2025 double-blind randomized trial1 and a Cochrane review of 7 trials3 both point toward real, measurable benefits.
Table of Contents
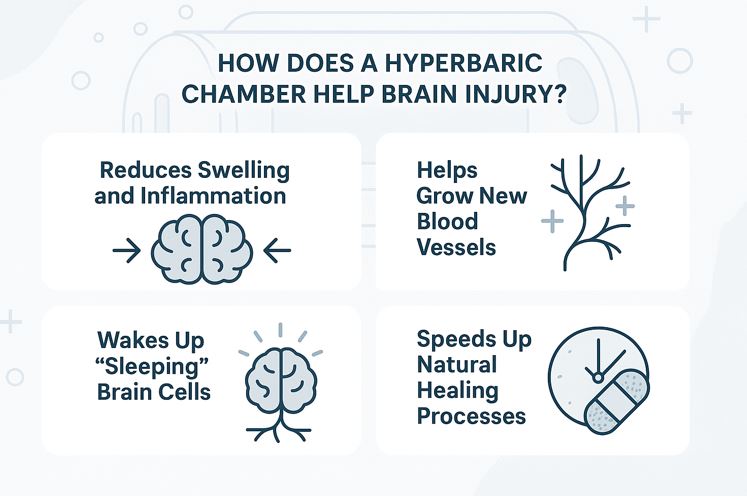
How Does a Hyperbaric Chamber Help Brain Injury?
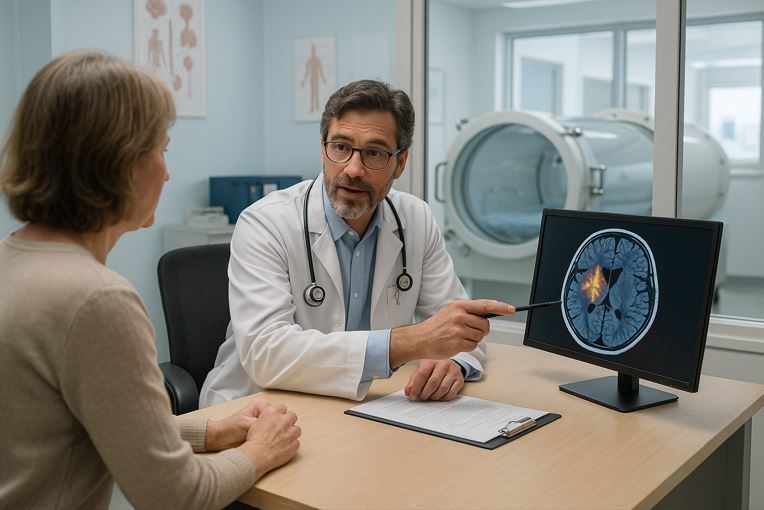
Think of your brain like a car engine that’s been in an accident. Some parts work fine, but damaged areas aren’t getting enough fuel to run properly. A how HBOT works for brain injury fixes this problem by flooding your entire system with extra oxygen.
During each session, you lie in a chamber while breathing 100% oxygen at roughly 1.5 to 2.0 ATA (atmospheres absolute). The elevated pressure forces oxygen deep into your bloodstream and brain tissue, even reaching areas where damaged blood vessels have cut off normal supply.3
The extra oxygen helps your brain in several important ways. It reduces swelling and inflammation around injured areas. It helps grow new blood vessels to replace damaged ones. Most importantly, it can reactivate brain cells that are not working but are not completely dead either. Researchers call this the “ischemic penumbra” – cells in a kind of suspended state that respond to renewed oxygen delivery.4
Many patients describe it as giving their brain the boost it needs to start healing itself. The process isn’t instant, but over weeks of sessions, people often notice their thinking getting clearer and their symptoms improving.
What Does Research Say About HBOT for TBI?
The good news is that science backs up what patients are experiencing. Multiple studies show that hyperbaric oxygen therapy can help people with brain injuries, though results vary from person to person. For a detailed breakdown, read our latest research.
“In the largest double-blind trial to date, HBOT patients improved their neurobehavioral symptom scores nearly three times more than those receiving sham treatment (10.6 vs 3.6 points, p=0.01).”
Weaver et al., 2025, Scientific Reports
The Cochrane Review pooled 7 randomized trials with 571 patients and found HBOT reduced TBI mortality risk by 31% (RR 0.69, 95% CI 0.54-0.88, p=0.003), with a number needed to treat of just 7.3 A 2016 meta-analysis of 8 prospective studies confirmed a pooled GCS improvement of 3.13 points (95% CI 2.34-3.92, p<0.001).4
A 2024 RCT in moderate TBI patients added to this picture. After 10 consecutive daily sessions at 1.4 ATA, the HBOT group scored 14.37 vs 13.40 on the Glasgow Coma Scale at discharge (p<0.001) and showed significantly better outcomes at 3 months (GOS-E: 7.62 vs 6.40, p<0.001).2
A 2025 meta-analysis specifically tracking cognitive domains found HBOT improved memory (MD 10.13, p<0.00001), attention (MD 7.99, p<0.00001), executive function (MD 7.16, p=0.002), and information processing speed (MD 7.48, p=0.01) across 4 studies and 250 patients.5
Not everyone responds the same way. Evidence is stronger for acute moderate-to-severe TBI than for chronic mild TBI. The severity of your injury, how long ago it happened, and your overall health all play a role in outcomes.
“Patients receiving early HBOT after moderate TBI scored a full point higher on the Glasgow Coma Scale at discharge and maintained significantly better functional outcomes at 3 months.”
Chaturvedi et al., 2024, Asian Journal of Neurosurgery
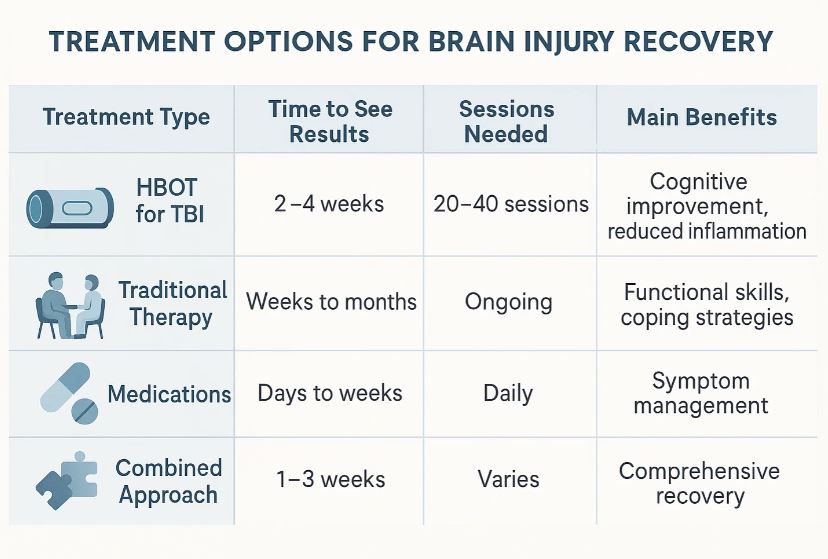
Treatment Process: What to Expect
Getting hyperbaric chamber therapy for brain injury follows a clear process. Before you start, you’ll need a complete medical evaluation and cognitive testing to measure your baseline abilities. Your doctor will also need to clear you medically to make sure HBOT is safe for you.
Most treatment protocols involve sessions lasting 60 to 90 minutes. You’ll typically go five days per week for a total of 40 sessions, depending on your specific needs. The chamber pressure usually runs between 1.5 to 2.0 ATA. Research suggests that 1.5 ATA protocols have consistently shown benefit in published trials for TBI, including the landmark Weaver 2025 study, while 2.0 ATA is used by the Efrati group for cognitive protocols.17
During each session, you’ll lie comfortably in a hard chamber and breathe normally while the oxygen does its work. Your ears might “pop” like on an airplane as the pressure changes. Many people rest, listen to music, or meditate during sessions. Most patients report no pain or discomfort.
Benefits You Might Notice
People getting hyperbaric chamber sessions for brain injury often report improvements in several areas. Your thinking and memory might become clearer, with less of that frustrating “brain fog” that makes everything feel difficult. Many patients find they can remember names, faces, and recent events better than before. For a deeper dive, check out our mental health applications.
Concentration and focus often improve. Tasks that used to feel overwhelming might become manageable again. Mental processing speed can get faster, making conversations and decision-making easier. The 2025 Shahid meta-analysis showed significant improvements across all major cognitive domains – memory, attention, executive function, and processing speed – in a population of 250 TBI patients.5
Physical symptoms frequently improve as well. Headaches often become less frequent or severe. Sleep patterns typically improve. Some people notice better balance and coordination. Emotional well-being tends to improve too, with moods becoming more stable and anxiety reducing.
Treatment Comparison by TBI Type
| TBI Type | Evidence Level | Best Available Study | Key Finding |
|---|---|---|---|
| Acute severe TBI | Moderate-Strong | Bennett/Cochrane 2012 | Mortality benefit (NNT=7) |
| Acute moderate TBI | Strong | Chaturvedi 2024 | GCS +1 point at discharge, better 3-month outcomes (p<0.001) |
| Chronic mild TBI/PCS | Mixed | Weaver 2025 / Harch 2020 | Positive at 1.5 ATA; negative at 2.0 ATA in military trials |
| Military PCS | Weak-Null | Cifu 2014 | No benefit over sham at 2.0 ATA; VA/DOD recommends against |
| Pediatric PCS | Moderate | Hadanny 2022 | Significant cognitive and behavioral improvements (sham-controlled) |
Cost Analysis and Insurance Reality
Clinical sessions typically cost between HBOT session costs to $300 per session at medical facilities. A complete program can run anywhere from $6,000 to $18,000 for a full course. Some people consider buying home chambers, which range from $15,000 to over $100,000, but soft chambers at home do not deliver the same therapeutic pressure as medical-grade hard chambers, and no published TBI research has validated their use.
Here’s the reality about HBOT insurance coverage. Most insurance plans don’t cover HBOT for brain injury because they consider it off-label. Veterans may have some coverage through VA benefits, and workers’ compensation sometimes covers it if the injury happened at work.
Don’t assume insurance will cover this. Get written pre-authorization before starting any program. Many treatment centers can help you check your benefits and explore payment options, but be prepared to pay out of pocket for most or all of the cost.
What Are the Side Effects and Risks?

Hyperbaric oxygen therapy remains among the safest medical procedures available, but like any medical intervention, it has some risks to consider. The Cochrane Review found that pulmonary impairment occurred in 13% of HBOT patients vs 0% in controls, so supervision matters.3 Most side effects are minor and temporary.
Common side effects include ear pressure or mild discomfort, similar to what you feel when flying. Some people experience temporary vision changes, usually minor and reversible. Fatigue after sessions is normal, and some people feel claustrophobic in the enclosed chamber.
Serious risks are rare but possible. People with lung problems could experience a collapsed lung. Those with seizure disorders might have an increased seizure risk. Fire risk exists because oxygen makes everything burn faster, which is why strict safety protocols exist in hard chambers.
The only absolute reason to avoid HBOT is an untreated collapsed lung. Other conditions that make sessions risky include recent ear surgery, certain lung diseases, current upper respiratory infections, and some medications. Your doctor will review all these factors before starting.
Frequently Asked Questions
Q: Can HBOT help old brain injuries?
A: Yes. Research shows that even brain injuries from years ago can still benefit from hyperbaric oxygen therapy. The Boussi-Gross 2013 trial enrolled patients 1-5 years post-injury and found significant cognitive improvements that correlated with increased brain activity on SPECT imaging. Your brain retains neuroplasticity long after the initial injury.
Q: Does insurance cover hyperbaric chamber therapy for brain injury?
A: Coverage varies widely. Some insurance plans cover it for certain conditions, while others don’t. Many treatment centers can help you check your benefits and explore payment options.
Q: How long do the benefits last?
A: Most studies show that improvements from HBOT can last months after sessions end. The Harch 2020 trial found improvements persisted at least 2 months post-treatment. Some patients do periodic sessions to maintain gains.
Q: Can I combine HBOT with other options?
A: Absolutely. HBOT often works best when combined with traditional therapies like physical therapy, occupational therapy, and counseling. The Chaturvedi 2024 trial used HBOT as an adjunct to standard care, not as a replacement.
Q: Is it safe for children with TBI?
A: HBOT has been studied in children. A 2022 sham-controlled trial found significant cognitive and behavioral improvements in children aged 8-15 with post-concussion syndrome.6 Pediatric brain injury specialists should be involved in any decision.
Conclusion
Hyperbaric chamber therapy for brain injury offers real hope for people who thought they’d reached the limits of their recovery. While it’s not a miracle cure, the growing research and patient success stories show it can be a powerful tool in your recovery toolkit.
The key is working with qualified professionals who can evaluate whether HBOT is right for your specific situation and coordinate it with your other treatments. For many families dealing with TBI, hyperbaric oxygen therapy has provided improvements they didn’t think were possible – giving back cognitive function, reducing symptoms, and most importantly, returning hope for a better future.
“Pooled analysis from the Cochrane Review found HBOT reduced TBI mortality risk by 31%, with a number needed to treat of just 7 – meaning for every 7 patients treated, one additional life is saved.”
Bennett et al., 2012, Cochrane Database
Who Should Not Try HBOT
HBOT is generally safe when administered by trained professionals, but it is not appropriate for everyone. Discuss your full medical history with your provider before starting.
Absolute Contraindications
HBOT should not be used if you have:
- Untreated pneumothorax (collapsed lung) – pressure changes can worsen this condition and become life-threatening
- Certain chemotherapy drugs – bleomycin, cisplatin, doxorubicin, and disulfiram may interact dangerously with high-oxygen environments
Relative Contraindications
Your provider may need to take extra precautions or postpone if you have:
- Upper respiratory infection or sinus congestion – difficulty equalizing pressure can cause ear or sinus barotrauma
- Seizure disorder – high-pressure oxygen can lower seizure threshold in susceptible individuals
- Chronic obstructive pulmonary disease (COPD) – altered breathing drive may require modified protocols
- High fever – increases the risk of oxygen toxicity
- History of ear surgery or chronic ear problems – pressure equalization may be difficult or risky
- Claustrophobia – may require sedation or use of a multiplace chamber instead
- Pregnancy – insufficient safety data exists for routine use during pregnancy
Talk to Your Doctor First
Even if you do not have the conditions listed above, always consult your physician before starting HBOT, especially if you take insulin, have a pacemaker or implanted device, or are currently taking any medications. For a full overview of HBOT side effects and risks, see our detailed guide.
References
- Weaver LK, Ziemnik R, Deru K, Russo AA. “A double-blind randomized trial of hyperbaric oxygen for persistent symptoms after brain injury.” Scientific Reports. 2025;15. DOI: 10.1038/s41598-025-86631-6
- Chaturvedi J, Mago V, Gupta M, et al. “Hyperbaric Oxygen Therapy in Moderate Traumatic Brain Injury: A Randomized Controlled Trial.” Asian Journal of Neurosurgery. 2024. DOI: 10.1055/s-0044-1791997
- Bennett MH, Trytko BE, Jonker B. “Hyperbaric oxygen therapy for the adjunctive treatment of traumatic brain injury.” Cochrane Database Syst Rev. 2012;12:CD004609. DOI: 10.1002/14651858.CD004609.pub3
- Wang F, Wang Y, Sun T, Yu HL. “Hyperbaric oxygen therapy for the treatment of traumatic brain injury: a meta-analysis.” Neurological Sciences. 2016;37:693-701. DOI: 10.1007/s10072-015-2460-2
- Shahid S, et al. “HBOT for neurocognitive deficits following TBI: a systematic review and meta-analysis.” Annals of Medicine and Surgery. 2025. DOI: 10.1097/MS9.0000000000003902
- Hadanny A, et al. “Hyperbaric oxygen therapy in children with post-concussion syndrome.” Scientific Reports. 2022;12:15233. DOI: 10.1038/s41598-022-19395-y
- Raj S, et al. “Role of HBOT in TBI: A Systematic Review of RCTs.” Indian Journal of Neurotrauma. 2024. DOI: 10.1055/s-0044-1782609
- Biggs AT, Dainer H, Littlejohn LF. “Effect Sizes for Symptomatic and Cognitive Improvements in TBI Following HBOT.” J Appl Physiol. 2021. DOI: 10.1152/japplphysiol.01084.2020
Medical Disclaimer
The content on BaricBoost.com is for informational purposes only and is not intended as a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.
Why Trust Our Evaluations
Our rankings are based on hands-on testing, published clinical data, and verified manufacturer specifications. We apply the same criteria to every product regardless of affiliate status. Editorial Process · Evaluation Methodology